CommercialDecember 1, 2021
Submitting prior authorizations is getting easier
You may already be familiar with the Availity multi-payer Authorization app because thousands of providers are already using it for submitting prior authorizations for other payers. Anthem Blue Cross and Blue Shield (Anthem) is eager to make it available to our providers, too. On December 13, 2021, you can begin using the same authorization app you use for other payers. We hope to make it easier than ever before to submit prior authorization requests to Anthem.
ICR is still available
If you need to refer to an authorization that was submitted through ICR, you will still have access to that information. We’ve developed a pathway to access your ICR dashboard. You will simply follow the prompts provided through the Availity Authorization app.
Innovation in progress
While we grow the Availity Authorization app to provide you with Anthem-specific information, you can still access ICR for:
- Appeals
- Behavioral health authorizations
- FEP authorizations
- Medical specialty Rx
Notices in the Availity Authorization App will guide you through the process for accessing ICR for Reserved Auth/Appeals functions.
Training is available
If you aren’t already familiar with the Availity Authorization app, training is available.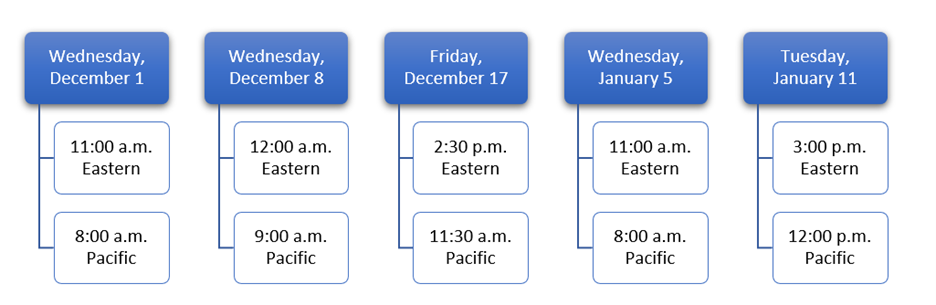
You can always log onto Availity.com and view the webinar at your convenience. From Help & Training select Get Trained to access the Availity Learning Center. You can use “AvAuthRef” for a keyword search or select the Session tab to see all upcoming live webinars.
Now, give it a try!
Accessing the Availity Authorization app is easy. Just log onto Availity.com and the Authorization icon is on the home screen. You can also access the App through the Patient Registration tab by selecting Authorizations and Referrals.
To view this article online:
Or scan this QR code with your phone
